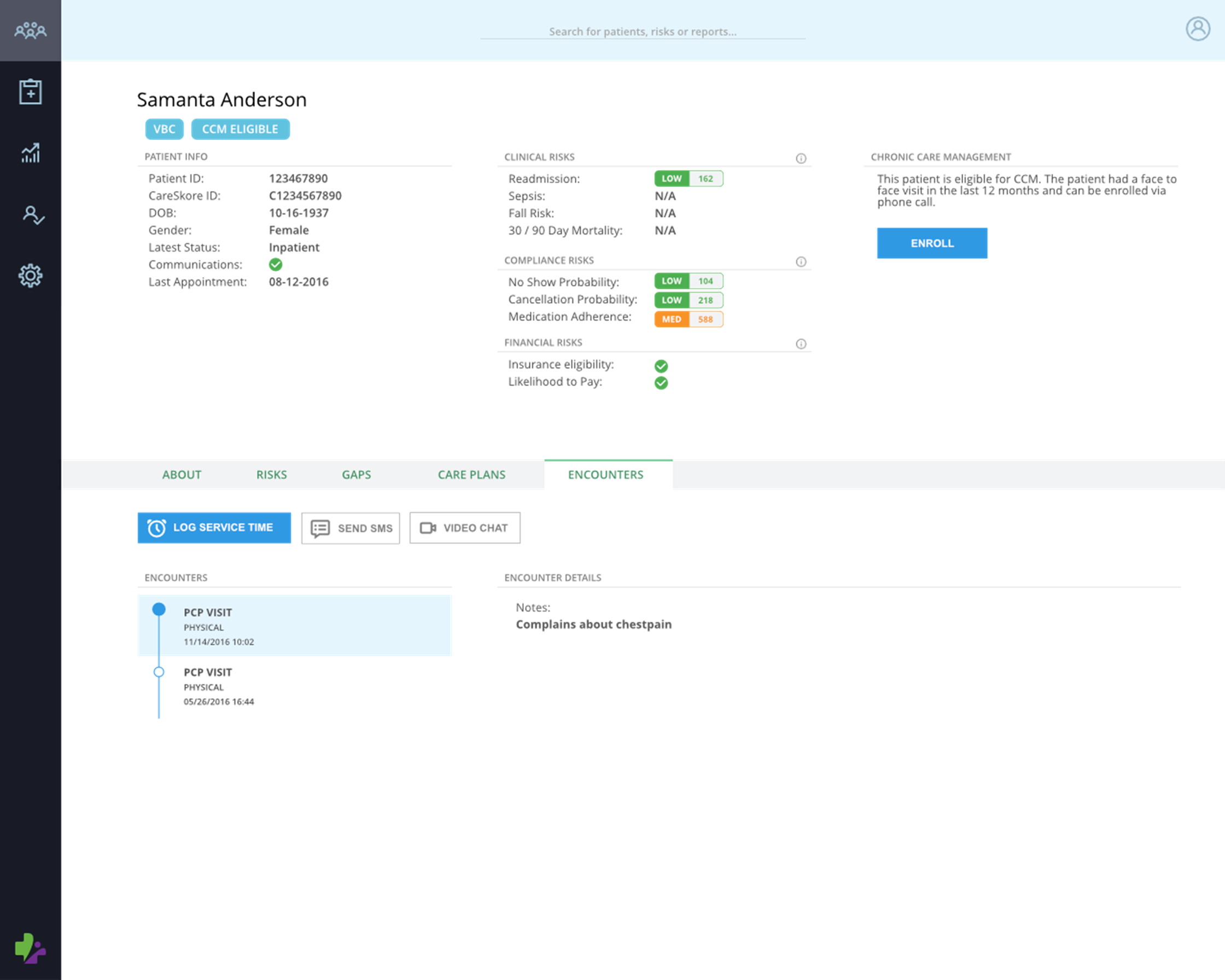
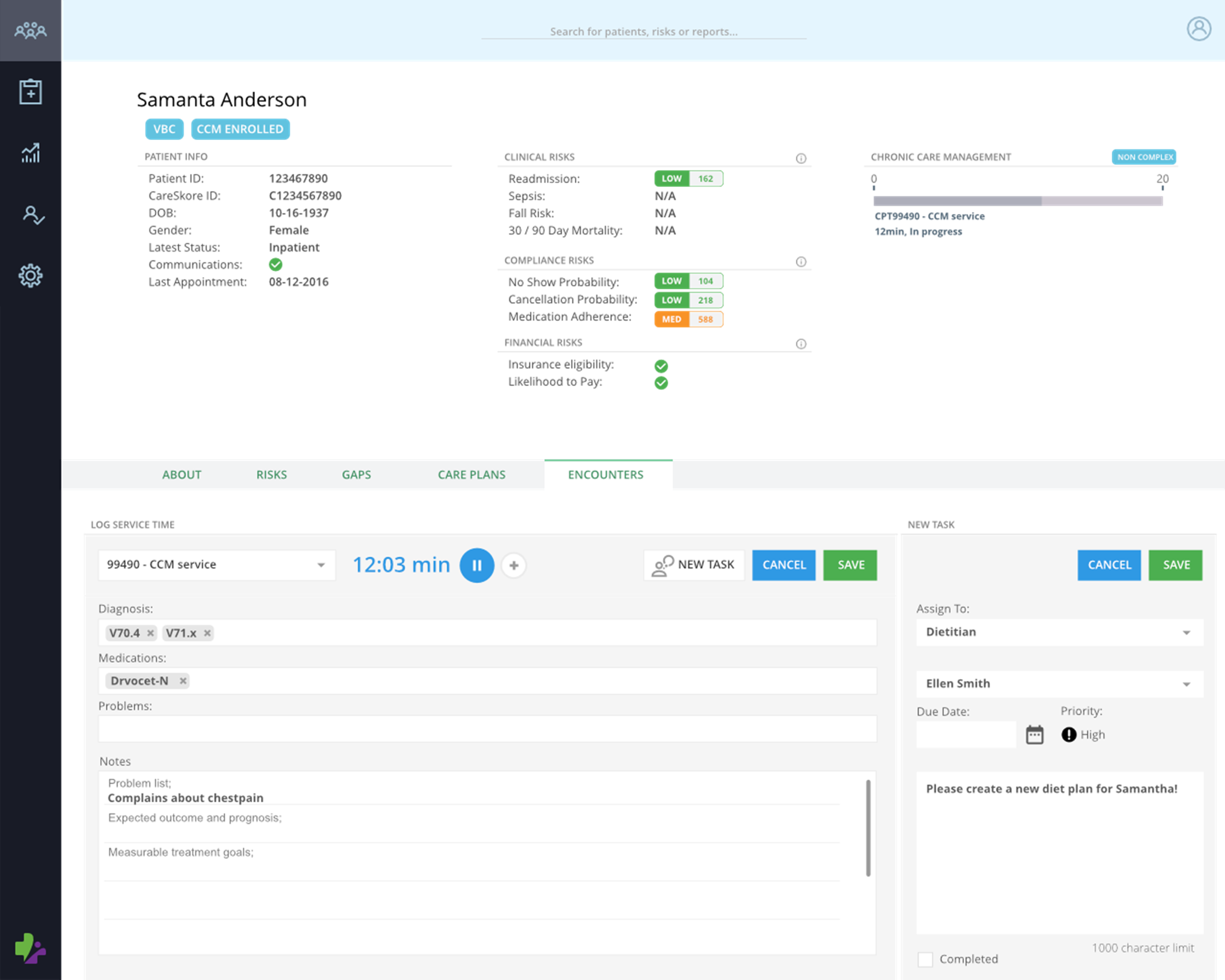
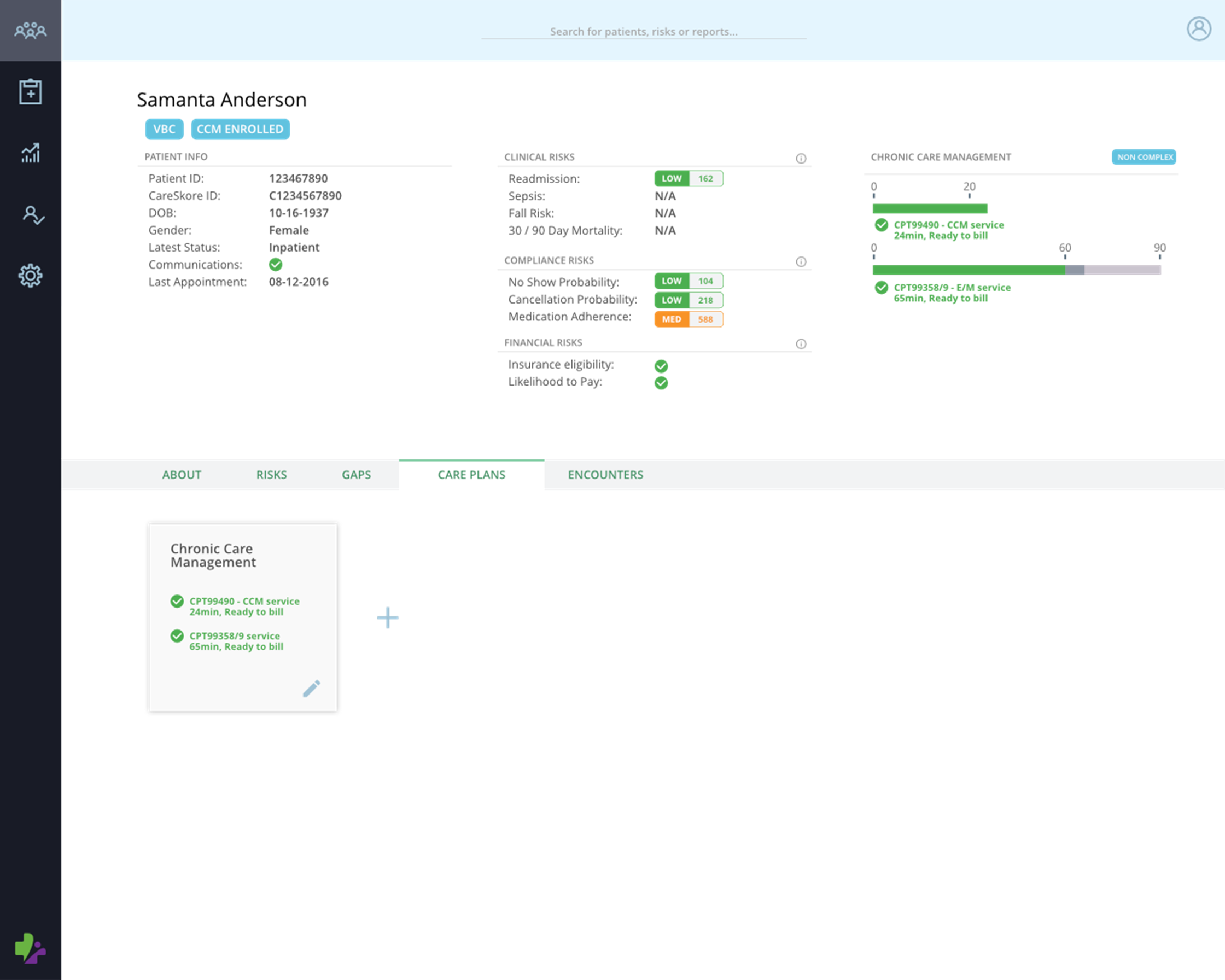
Chronic Care Management (CCM)
Manage and bill for eligible chronic care management (CCM) patients while optimizing care plans and automating patient engagement (includes all updates for 2017)
CCM Resources
Why CareSkore for chronic care management (CCM)?
-
Track time and bill against all current chronic care management (CCM) and complex chronic care management (complex CCM) billing codes
-
Quickly ID gaps in care plans
-
Automate workflows in patient care
-
Dynamically engage patients with AI-enhanced platform
Better manage patients with 2+ chronic diseases while maximizing reimbursements
With over 2/3 of the US population suffering from 2 or more chronic conditions, chronic care management (CCM) is becoming more and more prevalent.
CareSkore’s chronic care management (CCM) maximizes revenue while simplifying qualification, care plan development, workflows, and patient engagement.
-
Receive full reimbursement for all patient-related actions
-
Identify and auto-enroll chronic care management (CCM)-eligible patients early to reduce readmission risk.
-
Develop and get paid for care plans that reflect best-practices.
-
Engage chronic care management (CCM) patients for better outcomes while reducing per-provider patient loads.
Example Use Cases
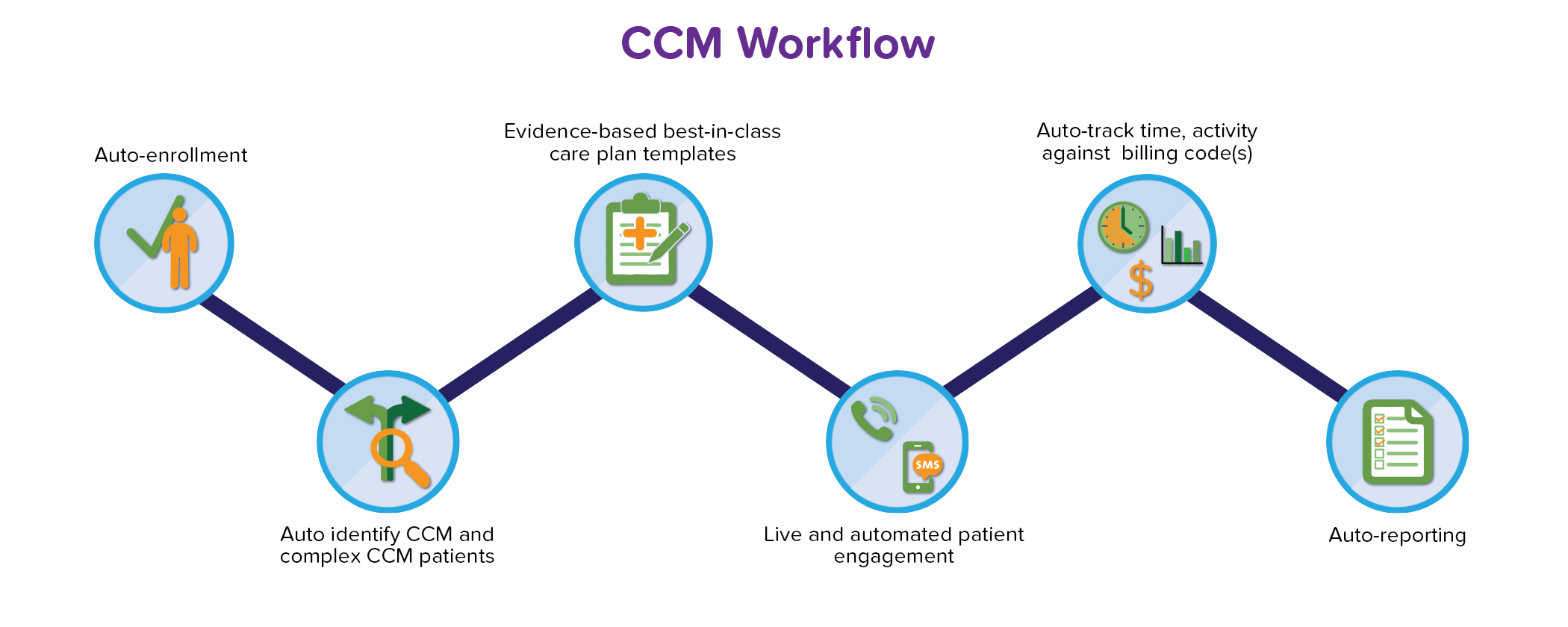
CCM Revenue Calculator Based on 2017 CCM Changes
Chronic Care Management Calculator
Estimate the potential revenue that any hospital can make by providing Chronic Care Management (CCM) to at-risk patients