It’s no secret that the shift to value-based is leading more physicians and nurses to be employed by hospitals. Patients feel the height of these effects because Medicare reimbursement rates have not yet kept pace with inflation. So how can physicians and nursing facilities manage their bottom line while losing money caring for this growing group of patients? Some will simply take care of fewer patients, which will reduce overall revenue in an effort to minimize the financial impact. However, there are things doctors and nurses can do to balance out the loss and actually improve margins during the slow transition to value-based care.
Overcome the Obstacles
First things first, you’ll need the right infrastructure and tools to make sure you’re accurately tracking all patients, so you can measure your performance and revenue. While this happens annually or quarterly, hospital CEOs and CFOs should be regularly accessing and evaluating this data in order to make continuous adjustments. Once you’ve synthesized all this information, you’ll want to rethink your traditional KPI’s (key performance indicators) associated with fee-for-service. Rather than focusing on traditional, one-dimensional metrics like headcount in beds or number of surgeries, you’ll need to get the full picture of your quality metrics. Instead, focus on metrics like:
- Cost per case
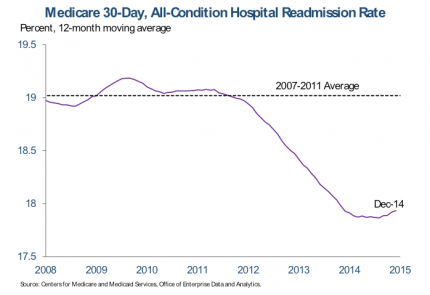
- Readmission rates
- Length of stay
- Complication rates
When you dive deeper into the data, you will probably find there are plenty of areas you can improve. Are there specific diagnoses codes that you struggle with? Are there other factors that contribute to readmission rates that might not be happening at your hospital?
Improve Care Coordination
Readmission rates are a major metric that is evaluated by CMS. However, even if you provide the best care, a patient could still be readmitted because they aren’t following up with their primary care provider. Skilled nursing facilities and home health solutions are also important factors to evaluate the quality of a patient’s care after they leave your hospital. Choosing the right partners and holding them to a high standard will help lessen readmissions and provide better continuity of care.
Become More Efficient
In come cases, you might find that the length-of-stay is longer for patients that receive an MRI, for example. If you only have one MRI for both inpatients and outpatients, your teams may be prioritizing outpatient diagnostic tests simply to accommodate business hours. But that leaves inpatients to wait until evening (around 8 pm) to get their MRI, which increases overall length-of-stay.
Other Strategies to Optimize
1. Expand access points
Free-standing ERs; outpatient diagnostic centers and urgent care facilities can all increase your volume of services you provide without the additional costs and potential penalties from inpatient stays.
2. Telehealth technology
Physicians or nurses that travel between hospitals, practice offices, and outreach. Clinics can reduce travel time and see more patients through virtual visits. Offering convenient telemedicine services can also be a market differentiator and attract more patients with commercial insurance that prefer the convenience of virtual visits.
3. Focus on specialization
By developing signature services you can focus on recruiting top-notch physicians and creating centers of excellence. Especially for procedures like joint replacement and bariatric surgery, you will draw patients that are potentially willing to pay more for a unique, high-quality experience. Ultimately, all of these efforts will result in better access to high-quality care for your patients, which will improve your composite scores and increase reimbursement potential.